Call Us
by Adam Brown
updated July 17, 2020
Sciatica is not a single diagnosis but rather a blanket medical term used to describe an entire set of symptoms that arise when one or more of the nerves that exit the low back are irritated or compressed. It is characterized by leg and buttock pain, and may also include numbness, tingling, or weakness of the affected leg. The problem is usually unilateral (on only one side), but in rare cases both legs can be affected. While many cases involve low back pain, others may not.
Sciatica Pain, and other Symptoms of Sciatica
While low back pain is common among Canadians, with an estimated 80% of the population set to experience the condition at some point in their lives, only about 5% of these cases involve symptoms that could properly be described as sciatica. Also, people aged 30-50 are more likely to develop sciatic pain.
What does sciatic nerve pain feel like?
It’s really painful. The pain, numbness, tingling, and profound weakness a person experiences depends upon exactly which nerves are affected, and where they are being compressed or irritated. Symptoms vary widely because of the many different conditions and separate diagnoses that are often lumped together and described as sciatica, but most common condition that most people describe is an intense back pain that runs down the length of the back and continues on down on what feels like the outside of the leg, from the buttock region to the foot and toes.
In most cases people are able to find a rest position that will minimize the intensity of their pain, while other positions may be consistently irritating to the condition.
What causes sciatica?
Any problem that compresses, inflames, or irritates the lumbar nerve roots or sciatic nerve, the large nerve bundle that passes through the buttock region, can produce symptoms described as sciatica. With this in mind there’s really no way to comprise any type of list but you’ll hear people complain about a new or old mattress, a long car drive, a new chair, a strange couch and any one of these elements may directly or indirectly cause the aforementioned compression or inflammation that results in the nerve bundle being irritated.
How a pinched sciatic nerve happens:
1) Lumbar disc bulge / herniation 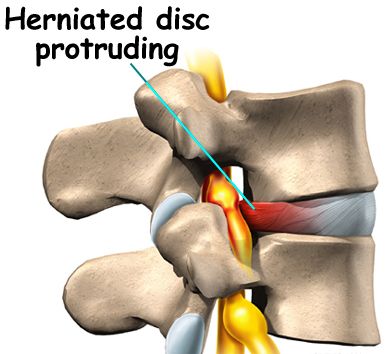
2) Foraminal stenosis 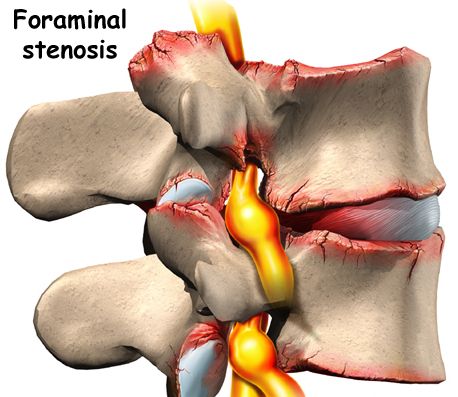
3) Spondylolisthesis 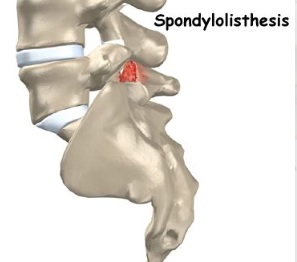
4) Piriformis syndrome 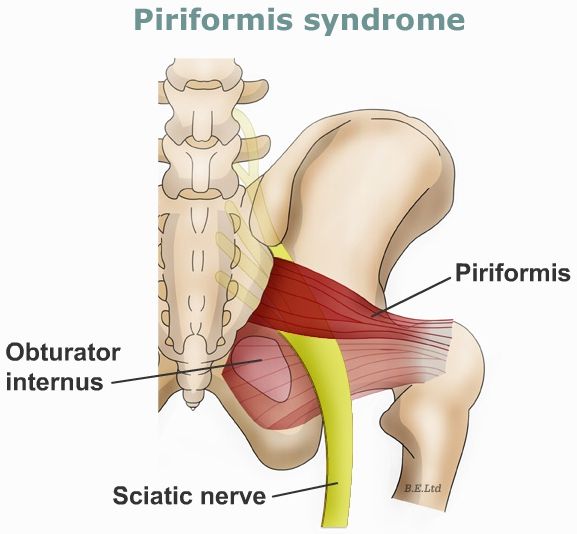
5) Central stenosis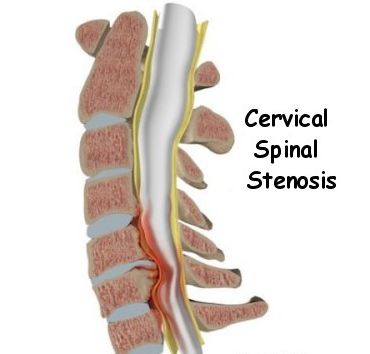
How is Sciatica Diagnosed?
It’s important to consult an experienced clinician for an accurate diagnosis of what is causing your sciatic symptoms. Each of the causes above should be understood and treated differently for best results. Diagnosis is made with a thorough history and clinical exam. You can help your clinician by thinking about what positions or activities always make your leg symptoms worse, and which ones seem to consistently provide relief. Provided the exam reveals a pattern of signs and symptoms consistent with sciatica, and there are no indicators of more serious pathology, there is usually no need for further tests, such as an MRI or X-ray.
Sciatica Treatment
Physiotherapy is the cornerstone of conservative care for sciatica. Treatment should be tailored to the specific cause of the sciatic symptoms, and will include some form of physical exercises to be done regularly. These may be aimed at improving spinal mobility, strength, or endurance. Treatment may also include manual (hands on) therapy, supervised exercises, or pain-relieving techniques like acupuncture.
An experienced physiotherapist can also consult on what activities are to be avoided while your symptoms are present, and teach you how to remain as active as possible without worsening your condition. They may also discuss Cognitive Behavioral Therapy (CBT) which can help manage chronic pain by training people to react differently to their pain.
As well, a doctor may prescribe medications to help ease symptoms and allow you to function better while you work on rehabilitating your sciatica. These medications may include anti-inflammatories, pain relievers, or drugs specifically tailored to relieve nerve pain.
Exercises for Sciatica
It’s important to note that for an exercise program to be maximally effective, it must be designed to address your specific type of sciatica. That being said, here are a few things that readers can try and which many patients report helping relieve their pain.
- Get moving! Even though you have pain, do not spend the day in bed. This tends to make things worse. Start by simply walking for a few minutes at a time and try to increase your distance slowly over time.
- Avoid sitting for long periods of time. And if you must sit use excellent posture in a good supportive chair. Many people with symptoms of sciatica find that their leg pain is much worse after sitting continuously for longer than 20 min.
- Child’s Pose For many patients this position will help to temporarily relieve their leg symptoms while not aggravating their back condition.
How long does sciatica last?
Thankfully, most cases of sciatica resolve with conservative treatment within 6-12 weeks. However, most people who have had an episode of sciatica will also have a recurrence at some point in the future. You can talk with your doctor and your physiotherapist about how to minimize future recurrences.
We can help.
If you are suffering from sciatica and are in the Toronto or Burlington area, book an assessment with one of Cornerstone’s experienced physiotherapists by calling our physiotherapy clinics at (416) 595-5353.

Questions? We're happy to help!
Choosing the right service provider can be a big decision. We’re dedicated to answering any questions you have to help you make the best choice. Contact us today and ask us anything!
Call us at (416) 238-6749




