Call Us
by Melissa Seifried and Giacomo Silvestri
Long COVID Physiotherapists
updated July 15, 2021
The Information and Breathing Exercises You Need to Fully Recover
Many people are not aware that physiotherapists are educated in the cardiovascular and pulmonary systems and are trained to aid the improvement of lung function in patients suffering from a variety of respiratory conditions. It is with this knowledge and a desire to help those directly impacted by COVID-19 that we have created this resource. It seeks to help those who have been diagnosed with Long Haul COVID and are currently recovering at home. This article will outline the basic function of the respiratory system, the anatomy and mechanics of the lungs, as well as provide recommendations to improve respiratory health.
Click here for our Guide to Long Covid (Long Haulers)
How the Respiratory System Works
When it comes to the mechanics of breathing, the respiratory system is made up of several components, all of which serve a vital role in effective breathing. The respiratory system functions to bring oxygen into and remove carbon dioxide from the muscles and organs in your body.
ANATOMY OF THE RESPIRATORY SYSTEM
1. Airways
The upper airway is made up of everything from your nose to the trachea, which is a cartilage tube that connects your mouth and nose to your lungs. The lower airway on the other hand is a system of conducting tubes which allows air to travel to the deepest part of the lung to bring in oxygen. This includes some of the larger tubes like our bronchi (think bronchitis) all the way down to the smallest of these tubes called the respiratory bronchioles.

2. Muscles of Inspiration (Breathing In)
The Diaphragm is a dome shaped muscle that is the major driver of inspiration, or breathing in. When you breathe in, your Diaphragm contracts and flattens out, pulling your lungs down and filling them with air. When you breathe out, the diaphragm relaxes and it allows air to escape from your lungs into the environment.
When we are breathing at rest, the diaphragm does most of the work when it comes to breathing in. If someone is working harder to breathe (for example when exercising or they are sick) our body recruits more muscles that help with breathing in. These include the: External Intercostals, Sternocleidomastoid, Scalenes, Pectoralis Major and Minor, Trapezius and Erector Spinae.
3. Muscles of Expiration (Breathing Out)
Unlike breathing in, expiration (or breathing out) is mostly accomplished by the elastic recoil of the lungs and rib cage. But when we require a forceful exhalation (for example when coughing or blowing out candles on a birthday cake) we can recruit our abdominal muscles to do so.
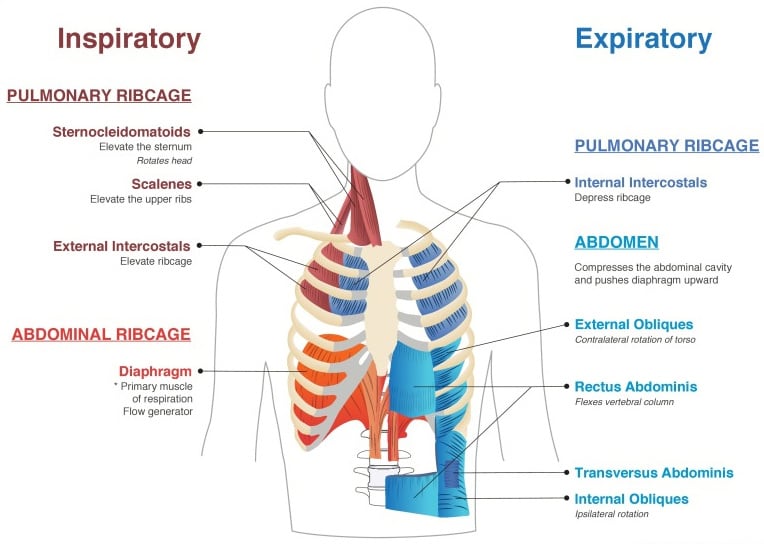
4. The Rib Cage (Thorax)
Along with protecting vital organs, your ribcage allows the muscles of respiration (breathing) to inflate and deflate your lungs effectively helping you breathe. The contraction and relaxation of these muscles moves your thorax which leads to air coming into your lungs during inspiration and out of your lungs during expiration.
PHYSIOLOGY OF THE RESPIRATORY SYSTEM
1. The Respiratory Cycle
When breathing in (inspiration), the respiratory muscle contraction leads to an increase in the size of the rib cage and air flow into the lungs. As we mentioned above, at rest this is mainly accomplished by the diaphragm. During exercise, the accessory muscles are recruited to help increase breathing rate and depth.
When breathing out, relaxation of the inspiratory muscles and the elastic relaxation of the lungs leads to an increase of pressure in your lungs and lets air flow out of your lungs.
2. Movements of Respiration
PUMP HANDLE MOVEMENT
During inspiration as your diaphragm contracts and flattens out, this leads to your chest moving up and forward like a water pump handle (see below). This is part of what helps your lungs expand and fill up with air. At rest, your chest returns to a relaxed position as the air is pushed out of your lungs through the elastic recoil of your rib cage.
BUCKET HANDLE MOVEMENT
This movement describes your ribs opening up when you take a deep breath in, and Increases slightly when your respiratory muscles contract. This causes the lower parts of your ribs to elevate in a bucket handle movement

How does COVID-19 / Coronavirus affect my lungs?
This particular novel coronavirus spreads via droplets expelled from an infected person through coughing, sneezing or exhaling air. Infection can spread regardless of whether or not an individual is symptomatic.(1) It is estimated that 80% of those infected will experience mild – moderate symptoms including cough, fever and shortness of breath.1 However, in more severe cases, the infection can lead to Pneumonia which causes inflammation in the tiny air sacs inside your lungs known as alveoli. This causes the lungs to fill up with fluid, making it even harder to breathe.(2) In even more severe causes, Pneumonia can lead to Acute Respiratory Distress Syndrome (ARDS).(3) You are at an increased risk of developing ARDS if you are older or have a history of tobacco use, alcoholism, chronic lung disease or have underwent a high-risk surgery.(3) Typically, patients are diagnosed with ARDS after already being admitted to the Intensive Care Unit (ICU).
How to use respiratory rate to assess your lungs following COVID-19 infection
New research from CQUniversity Australia and The Human Performance Company indicates an increase in breathing rate may be an early warning sign in the development of pulmonary disease including the Novel Coronavirus (COVID-19). Upper respiratory tract infections like a cold or the flu do not affect the respiratory rate, but lower respiratory infections, such as COVID-19, do have this association.
Breathing rate can be used to monitor your symptoms when recovering from COVID-19 or other lower respiratory tract infections. The easiest way to do this is to count how many times you breathe over a one-minute time span. A normal respiratory rate for an adult is 12-20 breaths per minute. As you recover from your infection you should expect your increased respiratory rate (a rate greater than 25 breaths per minute is considered abnormal) to return within the normal range of 12-20 breaths per minute.
Note that respiratory rate is both unconscious (it happens when you’re not thinking about it) or conscious (you can control your breathing rate). For this reason, it may be more accurate to have someone else measure your respiratory rate for you when you are not paying attention. This is only recommended if proper physical distancing can be maintained or if individuals are isolating as part of a group.
Pulmonary Rehabilitation – Physiotherapy to Improve Lung Function
The following recommendations to improve respiratory health and reduce exposure / re-exposure to viral particles are safe for individuals in reasonable health. Anyone with specific health concerns or pre-existing respiratory conditions should consult their physician before adopting them.
1. Rest
Many people who are suspected of having had the virus report fatigue or tiredness.(1) Your body is using more of its energy stores to fight a virus that is infecting the cells in your lungs. Even with mild symptoms, you could have some days when you feel fine and other days when you feel more tired and sore. When you are fatigued, stay home and rest as much as you are able.
2. Breathing Exercises
As this particular strain of novel coronavirus is still in its infancy, studies have not yet been conducted on the long term effects on patients’ lung health and function. It is thought that the virus causes inflammation around the alveoli of the lungs and reduces total lung capacity.(4) It is not clear if these changes are temporary or more permanent. Your lung capacity is defined as the total amount of air that your lungs can hold. Currently, there are no formal recommendations that patients who have recovered from COVID-19 should perform regular breathing exercises from the WHO. However, breathing exercises should be safe for those individuals who are not experiencing breathlessness. Breathlessness is defined as “uncomfortable, rapid or difficult breathing”. You should only try the exercises described below if you are in reasonable health and are not experiencing regular breathlessness. When performing the exercises, take 3-4 breaths at a time to avoid hyperventilation and resulting dizziness. It is also encouraged to breathe in through your nose to humidify the air entering your lungs and trap infectious particles. If you are feeling breathless while performing these exercises, stop them immediately and consult a physician.
The following exercises are recommended by the American Lung Association for basic pulmonary rehabilitation for a variety of respiratory conditions.(5)
A. Pursed-Lipped Breathing
Pursed-lipped breathing is used to slow your respiratory rate which allows your airways to stay open longer. This improves the rate at which you exchange gases between your lungs and blood vessels and makes the work of breathing much easier.
To practice the pursed-lipped breathing technique:
-
- Inhale slowly through your nose for a count of two.
- Purse your lips, as if pouting or blowing out candles.
- Breathe out as slowly as possible through pursed lips for four seconds.
*Note: If you are able to inhale for longer than two seconds, your exhale should take at least twice as long as the inhale did
-
- Repeat for 3-4 breaths and break for at least 30 seconds to avoid hyperventilation.
B. Diaphragmatic Breathing
Diaphragmatic breathing, or “belly breathing,” engages the diaphragm, which is supposed to be the primary muscle we use to breathe.
To practice diaphragmatic breathing technique:
-
- Sit in a supportive chair or lie down on your back with your knees bent and your feet on the floor.
- Your shoulders should be relaxed away from your ears.
- Place one hand on your belly and the other on your chest.
- Inhale deeply through your nose for two seconds, feeling the air move into your abdomen and feeling your stomach move outwards into your hand.
- Breathe out for two seconds through pursed lips while pressing on your abdomen.
- Repeat for 3-4 breaths and break for at least 30 seconds to avoid hyperventilation.
3. Lying Prone
Patients in the ICU suffering from COVID-19 are often placed prone, or on their stomachs, to help to synchronize the exchange of oxygen and blood flow in their lungs. Placing a person on their front can change the way blood and air flow through the lungs, which is ideal for patients suffering from respiratory viruses like the coronavirus. Data supports prone positioning to improve oxygenation and reduces mortality in patients with ARDS.(6) An ICU doctor in the UK recently recommended lying prone for 10 minutes a day with a pillow and performing slightly deeper breaths than your normal resting rate.(7) It is not recommended to lie on your front if you are in poor health, have mobility issues, or are pregnant.
Lifestyle Factors to Prevent Infection and Improve Lung Function
Stop Smoking
This shouldn’t be a surprise! We know smoking tobacco damages the lung tissue, among a host of other negative effects including a reduction of overall lung capacity. According to the Lung Association, your lung capacity can improve up to 30% within 2-3 months of quitting.(8) It can additionally be helpful avoiding open fires or secondhand smoke as much as possible.
Consume Enough Vitamin D
A population health study published in 2018 found that higher vitamin D levels were associated with better lung function.(9) With the current mandate to stay home as much as possible, you will likely not be getting enough Vitamin D from the sun. It may be worth investing in supplements but you should consult with your physician first. Vitamin D can also be found in foods such as fish, eggs and red meat. Visit health.gov for more food sources of Vitamin D.
Sing! Laugh!
A 2016 consensus paper concluded that singing has the potential to deliver health, psychological and social benefits to people with long-term respiratory conditions.10 Additionally, a 2015 study of 20 students found that the average lung capacity of choir singers was higher than that of non-singers.(11)
And although it might not seem like there is much cause for laughter these days, laughing is known to be great exercise for the abdominal muscles. It is thought to aid in clearing your lungs by forcing enough stale air out that it allows fresh air to enter into more areas of the lung.(12)
Improve Your Posture
Studies have shown that sitting in slouched postures decreases lung capacity.(13) This is thought to be due to the effect of the positioning of the ribcage on your lungs. So, for a very quick fix, imagine a string at the top of your head pulling you upright. Sit up straight to get the best lung capacity you can.
Improve the Air Quality in Your Home
If you live in a city, air pollution is unavoidable. Even short-term air pollution can decrease the function of your lungs.(14) But there are things you can do to improve the air quality at home. Dusting regularly and having certain house plants can help keep the air purified. You can also invest in portable air filtration systems for your living space.
Boost Your Immune System
Reducing your alcohol consumption, exercising regularly, getting consistent sleep and reducing stress in your life can aid in your immune function. Eating a balanced diet with more vegetables and fruit and less processed foods is also important for immune function.
Drink Plenty of Water
Staying well hydrated helps thin the mucosal linings in the lungs. When this lining is thinner, the lungs function better. The general recommendation for daily water consumption for adult females is 11.5 cups (2.7 litres) and 15.5 cups (3.7 litres) for adult males.(15)
Engage in Aerobic Exercise
Moderate daily aerobic exercise can improve lung function and support your immune system as well. Aerobic exercise is ideally done outdoors or inside with good ventilation. Longer walks or even jogging may improve lung capacity. Jumping jacks, jogging in place, or dancing can be done in smaller spaces like apartments. The current physical activity guidelines in Canada recommend that adults aged 18+ years should perform at least 150 minutes of moderate to vigorous physical activity per week.(16)
How to Know You Have Recovered from Pneumonia
Data from the American Lung Association suggests it may take time to recover from pneumonia, whether it is associated with COVID-19 or not. Some people feel better and are able to return to their normal routines within a week, while it can take a month or more for others. Studies suggest that most people continue to feel tired for about a month. These recovery benchmarks do not replace the consultation of a registered healthcare professional. Ensure that your primary healthcare provider has assessed you and cleared you for a full return to function.
Recovery Benchmarks
- Chest X-ray: a normal chest x-ray is often required to deem someone as recovered from Pneumonia
- Sputum Testing: your doctor may order sputum (mucous) testing to ensure any bacteria which may have been present when you were diagnosed, is no longer present in your system
- Pulmonary Function Tests: noninvasive tests that show how well your lungs are working. These tests measure lung volume, capacity, rates of flow, and gas exchange. Your healthcare provider may compare your values to age/sex predicted values and assess how well you have recovered.
References:
- https://www.who.int/news-room/q-a-detail/q-a-coronaviruses
- https://www.webmd.com/lung/covid-and-pneumonia#1
- https://www.lung.org/lung-health-diseases/lung-disease-lookup/ards
- https://www.webmd.com/lung/what-does-covid-do-to-your-lungs#1
- https://www.lung.org/lung-health-diseases/wellness/breathing-exercises
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4173887/
- https://globalnews.ca/news/6788251/breathing-technique-coronavirus/
- https://www.lung.ca/lung-health/smoking-and-tobacco/benefits-quitting/2-weeks-3-months
- https://www.ncbi.nlm.nih.gov/pubmed/29365367
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5131649/
- https://www.ncbi.nlm.nih.gov/pubmed/26482399
- https://www.lung.ca/blog/love-laughter-and-lungs
- https://www.ncbi.nlm.nih.gov/pubmed/16571389
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5471732/
- https://www.mayoclinic.org/healthy-lifestyle/nutrition-and-healthy-eating/in-depth/water/art-20044256
- http://csep.ca/CMFiles/Guidelines/CSEP_PAGuidelines_0-65plus_en.pdf


Melissa Seifried MScPT
Giacomo Silvestri MScPT
Melissa and Giacomo are both registered physiotherapists who work at Cornerstone’s downtown physiotherapy clinics. They have education in post-secondary respiratory anatomy and physiology and experience in cardio-respiratory rehabilitation settings.

Questions? We're happy to help!
Choosing the right service provider can be a big decision. We’re dedicated to answering any questions you have to help you make the best choice. Contact us today and ask us anything!
Call us at (416) 238-6749